 COVID-19 vaccine injection in arm
COVID-19 vaccine injection in arm
While the recent policy dialogue in Sub-Saharan Africa (SSA) focuses on vaccine supply and issues of financing, relatively little is known about the willingness to be vaccinated against COVID-19 within the population (a related blog post discusses some of the existing evidence). This knowledge gap is particularly glaring as the region is home to a staggering 433 million people living in absolute poverty and the pandemic clashes with already precarious livelihoods, ill-equipped public health systems, and high prevalence of comorbidities. As a result, large swaths of the population in SSA remain severely exposed without high vaccine coverage.
This blog highlights some key findings from a recent paper using cross-country comparable data from the LSMS-supported High-Frequency Phone Surveys on COVID-19 (HFPS) to study COVID-19 vaccine acceptance in six Sub-Saharan African countries. At a time when regular face-to-face data collection nearly came to a complete halt, the data allow for robust insights into vaccine acceptance in one of the world’s poorest regions. Based on large, nationally representative, pre-COVID sampling frames, estimated rates can adjust for a number of coverage and non-response biases and feature a rich set of individual and household characteristics to disaggregate the analysis.
High acceptance of a COVID-19 vaccine
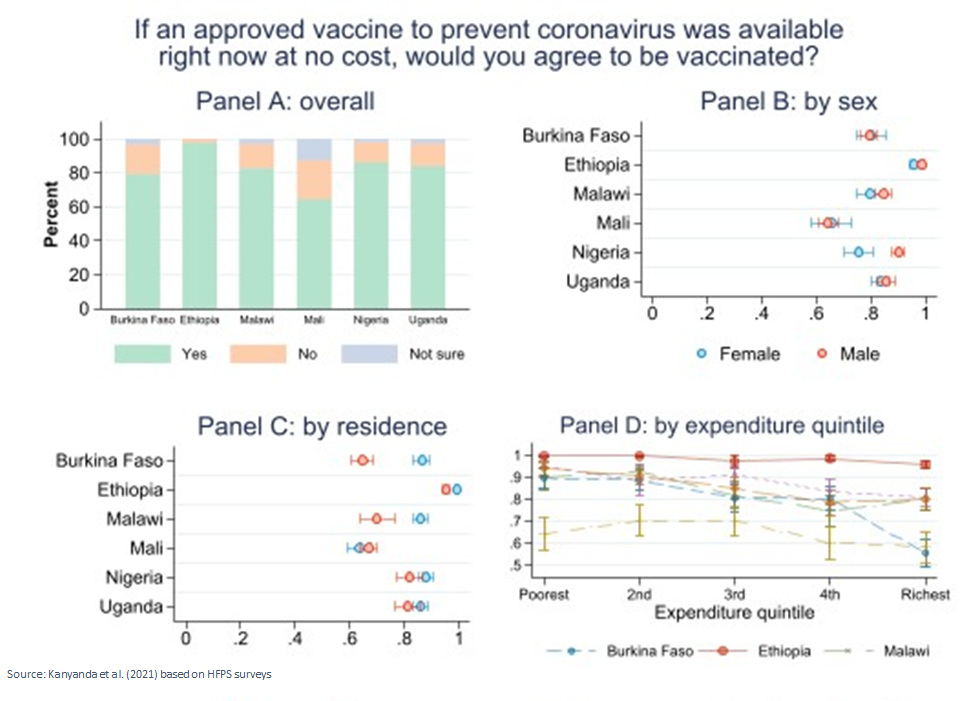
The data collected between September and December 2020 in Burkina Faso, Ethiopia. Malawi, Mali, Nigeria, and Uganda highlight high willingness to be vaccinated in these countries, before large scale vaccine rollouts had commenced. An estimated four in five people in all but one study country were willing to take an approved COVID-19 shot if it was made available to them for free. Acceptance rates exhibit some cross-country variation ranging from near universal acceptance in Ethiopia (97.9%) and high estimated acceptance in Nigeria (86.2%), Uganda (84.5%), Malawi (82.7%) and Burkina Faso (79.5%) to much lower acceptance in Mali (64.5%), a figure insufficient to reach the commonly stipulated threshold for herd immunity. A large share of the lower acceptance rates in Mali stem from more uncertainty among respondents with an estimated 12.4% stating they are unsure if they would be willing to be vaccinated.
Pockets of hesitancy in urban areas, among richer households and the better educated
Disaggregating acceptance rates reveals few systematic differences in vaccine acceptance by gender or age. However, estimates indicate some pockets of hesitancy in urban areas, among richer households, and those with higher levels of education. As these constitute groups that are likely easier to reach in the Sub-Saharan African context, resolving these clusters of hesitancy could be paramount to quick progression of vaccination campaigns.
Information and engagement campaigns promoting the safety of COVID-19 vaccines key
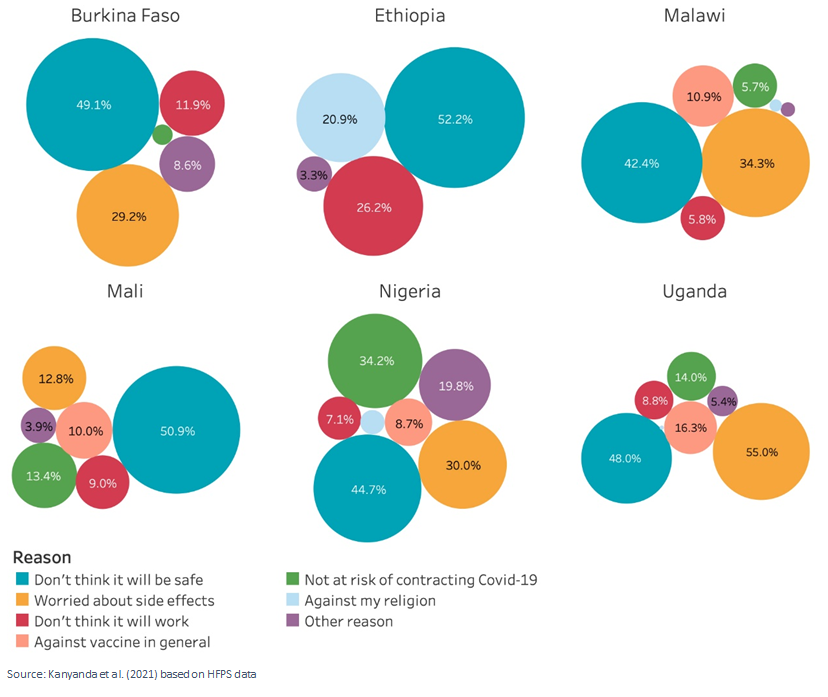
Among those hesitant to be vaccinated, concerns about the safety of COVID-19 vaccines and their associated side effects emerged as the primary reservations. Estimates suggest that close to half of those declaring to be unwilling to or uncertain about getting vaccinated in Ethiopia, Mali, Burkina Faso, and Uganda do not think that a vaccine would be safe. This is despite the question wording making it clear that the vaccine would be approved and may suggest high levels of distrust in the institutions involved in labelling the vaccines safe. Similarly, non-negligible shares of people worry about the side effects of the vaccines while their effectiveness or necessity is contested by fewer respondents. Information, sensitization, and engagement campaigns should thus put a special focus on strengthening confidence in the safety of vaccines and alleviating concerns about side effects.
Need to turn intent into effective demand
The results of a cross-country comparable study of vaccine acceptance in six Sub-Saharan African countries suggest high willingness to be vaccinated within the population. Therefore, inadequate demand likely does not present the key bottleneck to reaching widespread COVID-19 vaccine coverage in the region. As willingness to be vaccinated does not automatically translate to vaccine-seeking behavior though, public authorities will need to turn this intent into effective demand as the rollout progresses.
Targeting some clusters of hesitancy in urban areas, among richer households and those better educated could be key for a swift uptake of vaccination campaigns. In this regard, information and engagement campaigns should aim to bolster confidence in the safety of vaccines and resolve concerns about adverse side effects in order to reach mass coverage and also end the havoc the pandemic is wreaking in one of the world’s poorest regions.
Resources
- Read the full working paper including a discussion of the findings in relation to the literature
- Find out more about the LSMS-supported COVID-19 High-Frequency Phone Surveys





Join the Conversation