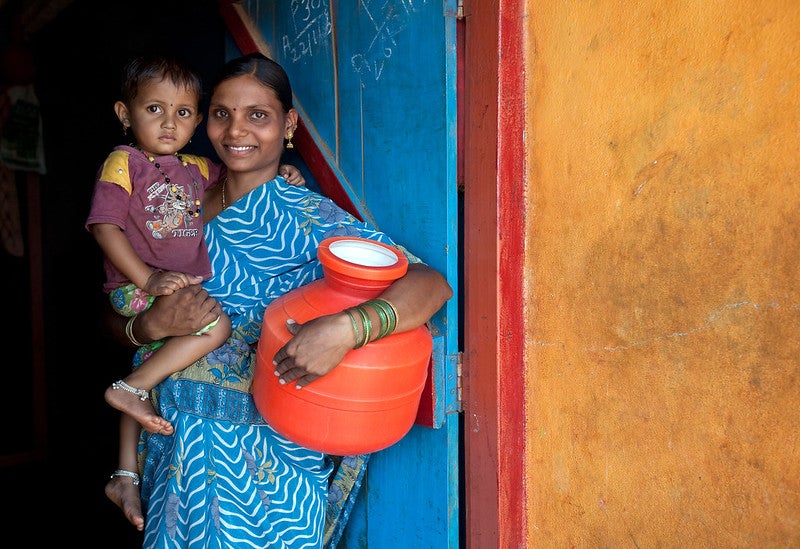 Geeta Bhogan (23) with her daughter Renuka at the family home in Bekkinakeri Village that she shares with family members and five cows.
Geeta Bhogan (23) with her daughter Renuka at the family home in Bekkinakeri Village that she shares with family members and five cows.
Malnutrition is a major public health issue in India. It affects children’s chances of survival, increases their susceptibility to illness, reduces their ability to learn, and makes them less productive in later life.
It has a wide range of causes, from the inadequate intake of food – especially too few calories and protein –to micronutrient deficiencies, inappropriate child-care and feeding practices, and poor hygiene and sanitation. Anemia and the low status of women also play a significant role as malnourished mothers are less likely to deliver healthy babies , perpetuating the cycle through the generations.
Evidence suggests that the most effective way of tackling a multidimensional challenge of this nature is by fostering strong collaboration between the various sectors and government departments that are charged to deal with the underlying issues.
While India’s Poshan Abhiyaan (National Nutrition Mission) seeks to address the issue on a nation-wide basis, a more intensive approach was piloted in two of the more isolated tribal areas in northern Karnataka.
Starting in 2014, the Karnataka Multisectoral Nutritional Pilot - supported by the World Bank and the Japanese Social Development Fund (JSDF) - focused on the Chincholi and Devadurga ‘blocks’ of Karnataka state where poverty ran deep and both malnutrition and anemia were persistently high.
Malnourished mothers are less likely to deliver healthy babies, perpetuating the cycle through the generations
The pilot’s success has generated interest among policy makers for replication in other parts of the country.
Six key strategies
The pilot adopted a few key strategies for maximum impact:
1. Adopted a multisectoral approach: To address the multiple causes of malnutrition, the pilot worked closely with ongoing government programs in health, education, and women and child development, as well as in water and sanitation. In every village, a nutrition volunteer was hired to work in conjunction with government functionaries on the ground, including front-line anganwadi workers (community nutrition workers) and accredited social health activists (Asha).
2. Targeted the most vulnerable households: The most vulnerable households were identified using India’s socio-economic and caste survey (SECC) of 2011. The survey is a more robust method of identifying vulnerability than the commonly used lists of people below the poverty line. The information thus gleaned was further corroborated through field visits.
3. Sought to address the intergenerational nature of the challenge: Since malnourishment often sets in before a girl becomes a mother and the nourishment a baby receives in the first thousand days of its life are critical for its future development, the project targeted three specifically vulnerable stages of the life cycle - adolescent girls, pregnant and lactating women, and children below three years of age.
4. Supplemented nutrition with locally-produced fortified foods: To boost the intake of calories and protein by women and children, high-quality, energy-dense food supplements were locally produced and distributed. The supplements - made out of local farm produce such as millets (ragi), chickpeas (gram), cane sugar (jaggery) and groundnuts - created a dent in the nutritional deficiencies commonly-found among the region’s people.
5. Spearheaded strong public awareness campaigns: Since changing age-old practices takes time and patience, the work of village volunteers was complemented by strong public awareness campaigns. Key messages were broadcast in three separate phases using different media streams, including radio and TV jingles. The messages were also painted on village walls.
6. Empowered women: Local women not only worked as village nutrition volunteers but were also employed in the manufacture of fortified food supplements. The women found it empowering to work for the betterment of their communities. They also learnt about the importance of looking after their own health which they tended to neglect, choosing to focus on their families instead.
Persistence pays
When village nutrition volunteers first went house-to-house to teach the largely illiterate families how best to care for mother and child, they faced many challenges. “At first, they would get irritated,” recalled a volunteer from Jalahalli village in Devadurga block. “But now they treat us like family.”
Families were taught how to improve the nutritional quality of their food while keeping within tight household budgets. The need to switch to iodized salt was also explained. “Earlier, I used to cook just rice and dal,” said a young mother from Jalahalli. “But after the volunteer visited us, we began eating nourishing food like millet, corn, and green leafy vegetables. I didn’t realize that the food we grow ourselves has so much nutritional value. ”
Creating synergies with other government programs
Importantly the project maximized the synergies with other government programs. For instance, volunteers reinforced the efforts of an ongoing health program that distributed iron tablets among school children by emphasizing the importance of taking these tablets , together with vitamin A supplements. The need to get timely vaccinations was also stressed.
A rural health worker from Devadurga block recalled the difference these efforts made. “Earlier, when iron tablets were given to pregnant women in hospitals, they used to spit them out thinking they could harm their baby. But now, people have understood their importance,” she said.
As bouts of diarrhea rob a child’s body of nutrients, the pilot leveraged the government’s ongoing Swachh Bharat Abhiyan, or Clean India Mission, to promote hygiene and sanitation. While the Mission helped construct over 2,600 toilets in the area, volunteers taught families how to maintain hygiene and treat diarrhea and school teachers were asked to reinforce these habits.
The pilot’s success has generated interest among policy makers for replication in other areas in India where stronger interventions are needed.



Join the Conversation