 A new tool can help measure job satisfaction of the health care workforce. © Dominic Chavez/World Bank
A new tool can help measure job satisfaction of the health care workforce. © Dominic Chavez/World Bank
Nurses, doctors, and other health care staff around the world have been voting with their feet.
Low job satisfaction has exacted a staggering toll on the profession, leading to resignations and staff shortages, compromising patients’ well-being, global health security, and the resilience of primary health care (PHC) systems.
And yet we know very little about the job satisfaction of the health care workforce, especially in low- and middle-income countries.
The World Bank’s Service Delivery Indicators (SDI) health team has a revamped, innovative survey that includes measurement of health care worker (HCW) job satisfaction—the first large-scale facility survey to capture this information. By measuring and then addressing workforce satisfaction, PHC systems can retain staff and, ultimately, improve the quality of care and health outcomes.
A long-standing shortage of health care workers
There has been a critical global shortage of HCWs, especially in low- and middle-income countries, for decades. In sub-Saharan Africa, there are only two doctors and 10 nurses for every 10,000 people—far below World Health Organization-recommended levels.
The world will need 80 million HCWs by 2030 but is projected to fall short by 18 million—with half the shortage in the nursing profession.
The COVID-19 pandemic has poured fuel on the fire.
Unsafe working conditions, including a lack of personal protective equipment, led to the death of as many as 180,000 HCWs between January 2020 and May 2021. Watching colleagues and patients succumb to COVID-19, along with other job stressors, drove many HCWs to quit.
In the United States, nearly one in five HCWs were part of the “Great Resignation,” a pandemic-related global trend across sectors that shows no signs of abating. In the Philippines, in just eight months in 2021, 7,000 nurses left for better jobs overseas. The brain drain there has reached critical levels.
The impact of burnout and stress
Health care is by nature a high-stress profession. But poor pay and difficult working conditions add to the strain of caring for ill or dying patients.
In low- and middle-income countries, HCWs often face poor health infrastructure and shortages of medicine and supplies. In Punjab, India, 75 percent of HCWs reported that they were dissatisfied with their working conditions.
Why does it matter?
HCWs suffering from burnout may make more medical errors, pay less attention to detail, take unnecessary risks, provide lower-quality care, and miss more days of work than satisfied employees.
In contrast, satisfied HCWs may be more motivated and productive, have fewer absences, enjoy better physical and mental health, and are likelier to stay on the job. It’s no wonder that some profitable companies put their employees first—they know that happy employees are likelier to treat their customers well, leading to repeat business and a better bottom line.
It is no different in health care, where HCW job satisfaction influences patient satisfaction and contributes to the continuity of care.
Revamped tool
The SDI health team has recently revamped its survey tool to comprehensively measure PHC service delivery—capturing not only health facility characteristics, but also the perspectives of patients and HCWs.
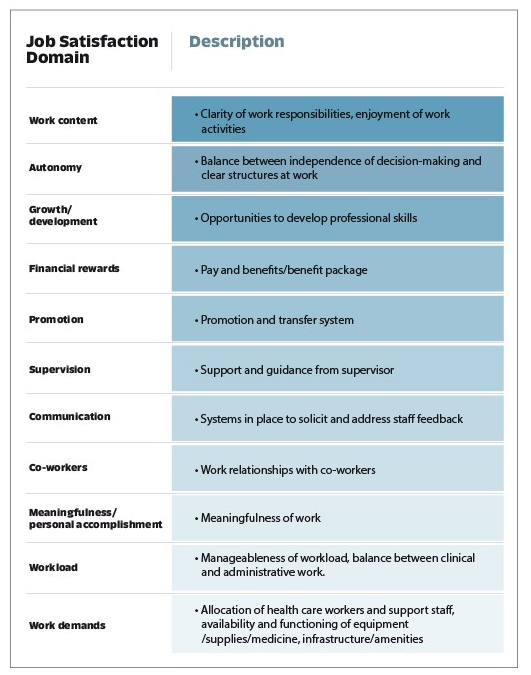
To determine how to incorporate questions about job satisfaction, we comprehensively reviewed the literature on best practices for measuring job satisfaction in general and among HCWs. To develop a streamlined yet comprehensive set of questions for the SDI survey, we used the framework outlined in one highly-referenced study to map the questions from frequently-used reliable and valid instruments onto common domains. (These instruments included the Job Satisfaction Survey, the Satisfaction of Employees in Health Care Survey, Emergency Physician Job Satisfaction Scale, Measure of Job Satisfaction Survey, and McCloskey/Mueller Satisfaction Scale.) We then generated questions to cover each domain of influencers of job satisfaction (table below), ensuring that they were applicable to all PHC HCW cadres, and used clearly defined terminology and consistent answer choices.
The revised SDI survey asks HCWs to say whether they agree or disagree, using a five-point scale, with a series of statements that capture these job satisfaction factors. For example, they are asked how likely they are to agree with the statement, “In my current role at this facility, my workload is manageable.”
This cutting-edge tool, which is being piloted in Moldova, Armenia, and Bhutan, holds promise to help PHC facilities learn where to intervene to take a people-centered approach to their workforces.
And if they do, it will pay enormous dividends—reducing burnout and the brain drain, improving health outcomes, building resilient health systems, and making progress toward achieving the Sustainable Development Goals.




Join the Conversation