 2 April 2020 - Cape Town, South Africa: Aerial view of empty streets in Cape Town, South Africa during the COVID-19 lockdown.© fivepointsix/Shutterstock
2 April 2020 - Cape Town, South Africa: Aerial view of empty streets in Cape Town, South Africa during the COVID-19 lockdown.© fivepointsix/Shutterstock
As of January 2021, the COVID-19 pandemic has claimed two million lives and infected almost 100 million people worldwide, and a devastating second wave of COVID-19 infections—accompanied with the emergence of multiple highly contagious mutant strains—is compelling governments to reestablish lockdowns and tighten social-distancing measures. Given the enormous personal and economic costs that coronavirus containment measures (CCMs) entail, policymakers need a detailed assessment of their effectiveness in containing the spread of COVID-19 and reducing its lethality. Two factors determine the effectiveness of CCMs: (i) the type of measures adopted, and (ii) the timing of their implementation and removal.
Using daily data for 158 countries from January to August 2020, our research reveals that CCMs have been broadly effective in slowing the spread of COVID-19 and reducing associated mortality. However, not all measures have been equally effective. Restrictions on activities, such as the closure of schools, workplaces, and international borders, appear to be more effective than restrictions on individual mobility and personal contact, such as stay-at-home orders or bans on private gatherings. In particular, closing schools and workplaces has had a strong containment effect. Adopting these CCMs would have reduced daily cases by around 6 to 8 percentage points 14 days after their implementation. While our findings are robust after controlling for the quality of national healthcare systems and other country characteristics, it should be noted that our research captures only the formal adoption of CCMs, and the effects in each country are likely influenced by unobserved variables related to compliance and enforcement.
Our research also shows that countries with more capable healthcare systems and warmer climates -- as indicated by higher minimum temperatures -- were slower to adopt CCMs, as these circumstantial factors tended to reduce the rate of spread, lessening the urgency of imposing more stringent containment policies. However, strong healthcare infrastructure and warmer climates only delayed the necessity of CCMs, and governments that put them off likely missed a valuable opportunity to lower their morbidity and mortality below the average for comparable countries. In addition, the results show that countries with more democratic institutions, as measured by the Economist Intelligence Unit’s democracy index, tended to adopt restrictions on activities in a timely manner, but were slower to implement CCMs limiting individual mobility and personal contact than countries with which populations did not observe as widely as those in more autocratic institutions. Importantly, the results detect demonstration effects, as the early adoption of CCMs in Western Europe led other countries to accelerate the implementation of their own measures.
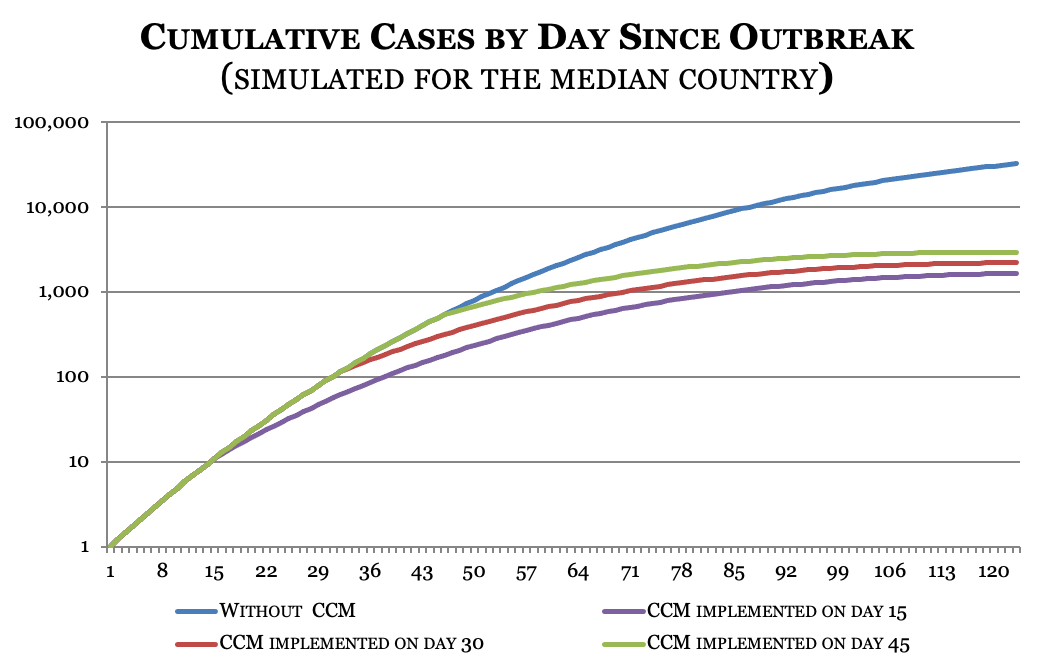
The findings of our research underscore the crucial importance of imposing and lifting CCMs in a timely manner. Predictions from the estimated models allow an assessment of the timeliness of adoption and lifting of CCMs by comparing the predicted timing for the introduction and lifting of CCMs with the actual timing of CCMs adoption in each country. Around 70 percent of countries in the sample closed their schools and public transportation systems at the optimal time predicted by the model. However, among restrictions on activities, border closures and the banning of public events were the slowest to be implemented, and just 55-60 percent of countries adopted these measures at the optimal (predicted) time. Moreover, just 30 percent of countries adopted measures restricting individual mobility or personal contact, such as stay-at-home orders and bans on gatherings, in a timely manner. The model also allows simulation of contagion and death rates in scenarios with different timings of adoption. In a baseline scenario in which no CCMs are adopted, the median country records more than 30,000 cases 120 days after the initial outbreak. If CCMs are implemented as late as 45 days after the initial outbreak, the number of cases falls to 3,000. If CCMs are adopted 30 days after the initial outbreak—the median lag—total cases fall to 2,200 after 120 days. Implementing CCMs just two weeks after the initial outbreak yields the best result, with total cases dropping to just 1,600 at the four-month mark. These large differences are explained by the interaction of two forces: adopting CCMs directly reduces the morbidity rate, and a smaller infected population reduces total morbidity through base effects. These complementary mechanisms are responsible for the massive differences in the evolution of the outbreak observed across scenarios.
Figure 1: Cumulative Daily Cases since the Initial Outbreak, Simulated for the Median Country
Finally, the evidence indicates that most countries resisted pressure to lift their CCMs too early. Over 60 percent of the countries in the sample kept their restrictions in place for as long as the model predicted was necessary. Nevertheless, around one-quarter of the countries terminated their CCMs one month or more before the time the worldwide evidence would have suggested was optimal. Stay-at-home orders and workplace closures were the CCMs most likely to be lifted early.
The findings of our research have clear implications for successfully crossing the ongoing second wave of the COVID-19 pandemic. Targeted restrictions on specific activities – rather than blanket shutdowns -- seem to be more effective in slowing down contagion and death rates and, as they face less resistance, these CCMs are also easier to implement in democratic contexts. Timely adoption and lifting of CCMs not only reduce the human cost of the pandemic but also enable a faster and more sustainable economic rebound.




Join the Conversation