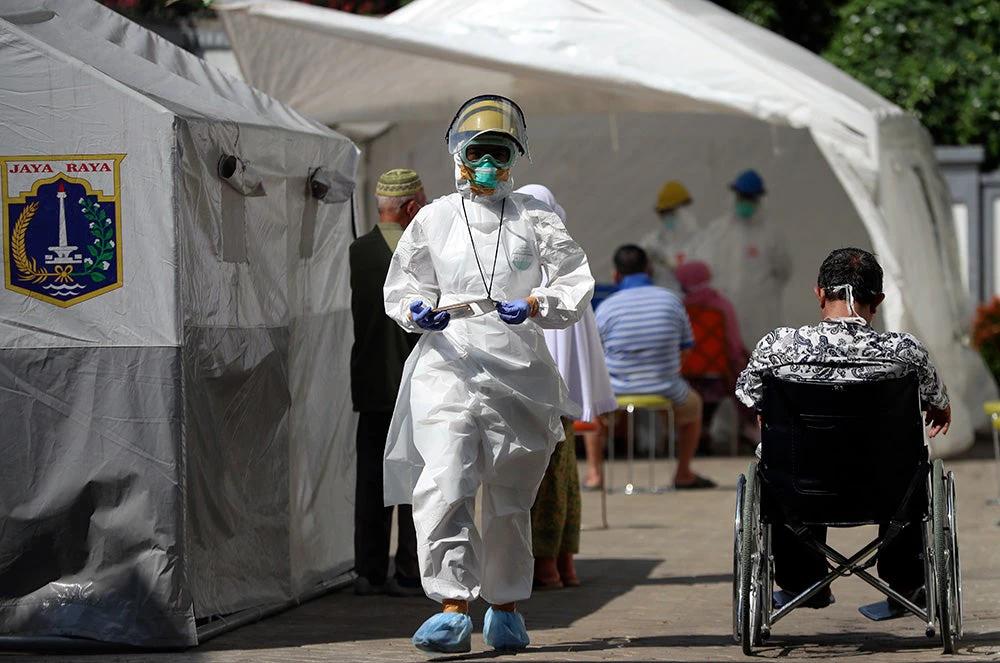
 2020年5月、新型コロナウイルス感染症大流行時のインドネシア・ジャカルタの地域医療センター。写真:Achmad / 世界銀行
2020年5月、新型コロナウイルス感染症大流行時のインドネシア・ジャカルタの地域医療センター。写真:Achmad / 世界銀行
On March 11 this year, the World Health Organization reported that the number of countries affected by COVID-19 had tripled in two weeks and declared the first pandemic caused by a coronavirus. Countries around the world moved swiftly to declare states of emergency, closing ports of entry and activating crisis management systems. Less than four weeks later, Tropical Cyclone Harold hit four Pacific Island countries, killing 27 people in Solomon Islands (resulting from a ferry incident) and damaging houses, infrastructure, and crops in Fiji, Tonga, and Vanuatu.
Such multiple and overlapping disaster and crises are demonstrating the need for adaptability and flexibility of national disaster risk management (DRM) systems , and how health-related emergencies are exacerbating existing vulnerabilities, and vice versa.
Some countries—including Korea, Singapore, and Vietnam—have applied lessons learned from Severe Acute Respiratory Syndrome (SARS) and Middle East Respiratory Syndrome (MERS) when responding to COVID-19. For example, these countries have improved disaster surveillance and disease outbreak alert systems (e.g., Singapore’s Disaster Outbreak Response System Condition) and maintained medical and emergency stockpiling.
Another key lesson learned by these countries was to establish a legal basis for inter-governmental cooperation in responding to health-related emergencies, allowing governments to make critical decisions swiftly , such as declaring a state of emergency and enacting travel and mobility restrictions.
By now, most countries have adopted a digital COVID-19 surveillance dashboard illustrating data and information such as case tracing and even geo-tagged local outbreaks (e.g., platforms in Indonesia and Myanmar). However, tracking infection rates, contact tracing, and case hotspots is not enough. There is limited integration of COVID-19 data with natural hazard data and risk information.
This will help to improve local- and community-level awareness and preparedness for disasters, encourage proactive emergency management (such as planning for a surge in medical and crisis management services), and updating local policies and guidelines for safe evacuation. For example, the government of Indonesia has disseminated a Guide for Tsunami Evacuation during COVID-19, which outlines special measures and protocols to mitigate and manage the pandemic risk.
Based on these early lessons, below are five ideas to consider when adapting DRM systems to address health-related emergencies:
- Review disaster risk management legislation, strategies, and policies. Enhance inter-agency coordination and integration of public health considerations in disaster management legislation and policy (and vice versa); and adapt multi-hazard approaches in DRM strategies and plans.
- Update national risk analyses and impact-based scenarios via a multi-hazard approach. Epidemiological forecast models could be incorporated into the decision support platforms to update multi-hazard risk modelling and identify areas vulnerable to concurrent risks – helping governments to target particularly vulnerable communities.
- Build on existing early warning systems for natural hazards and integrate alerts for health-related emergencies. Develop road maps for open data Multi-hazard Early Warning System platforms that integrate health surveillance and natural hazard information, and strong inter-agency coordination between Ministries of Health and National Disaster Management Organizations.
- Enhance community-based disaster preparedness programs to incorporate health-related emergencies. Community-based programs could incorporate preparedness for health-related emergencies – and help with case tracing, relief distribution, and public safety.
- Adapt emergency management systems to incorporate health-related emergencies. Update contingency plans and evacuation procedures and ensure that supply chains for relief/recovery goods and services are not disrupted.
A technical note on Adapting DRM systems for health-related emergencies was prepared with financial support from the Global Facility for Disaster Reduction and Recovery.
READ MORE:
- Technical Note: Adapting DRM systems for health-related emergencies: Early lessons from the Asia-Pacific region
Knowledge Note:



Join the Conversation