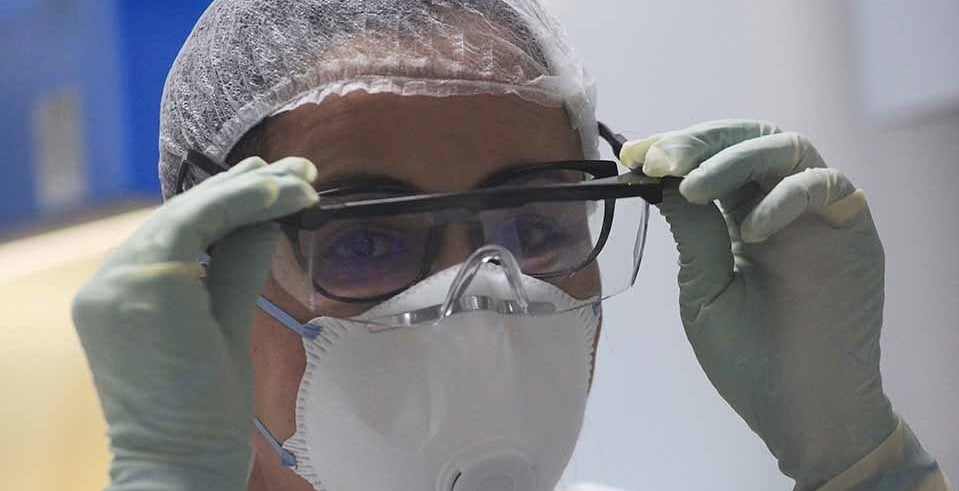
 A frontline health care worker in Morocco. © World Bank
A frontline health care worker in Morocco. © World Bank
May is observed as Mental Health Awareness Month in the United States. The COVID-19 (coronavirus) pandemic is placing greater focus on the importance of mental health as part of a comprehensive global response . A recently released UN policy brief, COVID-19 and the need for action on mental health, emphasizes that the pandemic aligns several mental health stressors: fear of contagion/dying, concern for health of family members, forced isolation due to quarantines, unemployment, and widespread financial distress. In addition, misinformation about prevention, non-stop exposure to pandemic-related news, and deep uncertainty about the future are further stressors that, collectively, could lead to a long-term global upsurge in mental health problems. Since the magnitude of COVID-19 is unprecedented, there are concerns that its mental health impact may be unprecedented as well.
This report highlights frontline health workers as being at particular risk. Reasons include:
- Emotional strain and physical exhaustion in caring for growing numbers of acutely ill patients and witnessing higher rates of mortality
- Anxiety around shortages of personal protective equipment, breakdowns of infection prevention and control protocols, and potential retaliation for speaking out about these concerns in public fora
- Concerns about infecting family members as a result of workplace exposure, sometimes leading to lengthy (voluntary) isolation away from support networks
- Difficult clinical decision-making on patient prioritization given limited availability of oxygen concentrators, ventilators, and other lifesaving medical equipment
- Anxiety on taking new clinical roles amid heavier workloads and longer hours
- The emotional toll of caring for coworkers who may become critically ill or die as a result of COVID-19
- Concerns about stigma as fear of the pandemic, amplified by misinformation, has resulted in frontline health workers being targeted for supposedly spreading the disease
- Limited access to mental health services for managing depression, anxiety, and psychological distress
Ensuring the mental health of frontline health care workers is critical in sustaining COVID-19 preparedness, response, and resilience. A few recent studies on the mental health of these personnel highlight a largely unmet need. In China, a survey of more than 1,200 health care workers providing COVID-19 care across 34 hospitals found higher levels of severe mental health symptoms than those in secondary roles, with high rates of depression (50%), anxiety (45%), and insomnia (34%). Other early studies indicate similar findings from countries as diverse as Canada (where 47% of health care workers reported a need for psychological support) and Pakistan (where 42% health-care workers reported moderate and 26% reported severe psychological distress).
Data from other epidemics, while limited, support similar concerns. A small study of health care workers during the 2003 SARS outbreak found that 89% of workers at high risk of contracting the virus reported negative psychological effects. Similarly, qualitative studies have documented negative mental health outcomes among health workers who fought Ebola in West Africa.
As the pandemic progresses, mental health symptoms will subside for some frontline workers but persist for others. Teletherapy and other virtual health services are crucial tools to sustain and strengthen their resilience. As they simultaneously provide care for patients and cope with occupational risk, it’s important to prioritize and monitor both mental and physical health needs of these workers over time.
Appropriate and timely mental health and psychosocial support can foster resilience, as some individuals will experience an increase in their own confidence and ability to manage future stressors. It can also help prevent mental health challenges. Early identification of risk and resilience factors, as part of a diagnostic approach, could be a key part of the crisis response.
Even when COVID-19 cases decline, the workload for frontline health workers is likely to remain heavy as health systems provide care that was unavailable or underutilized during the emergency response. There may be a continuation of higher morbidity and mortality following a decline in the pandemic, due to current disruptions in essential health services.
Global statistics on mental health were stark prior to the COVID-19 pandemic. Depression already affected 264 million people worldwide, and those with severe mental conditions are estimated to die 10-20 years earlier than the general population. In low- and middle-income countries, between 76% and 85% of people with mental health conditions receive no treatment despite evidence that effective interventions can be delivered in any resource context.
The World Health Organization has called for a scaling-up of mental health services in response to COVID-19, describing the pandemic as “an opportunity to build a mental health system that is fit for the future.” It advocates shifting care away from institutions to communities, ensuring coverage for mental health in health insurance packages, and building the human resource capacity to deliver quality mental health and social care.
The World Bank Group is supporting this global effort through its COVID-19 health sector response, in close partnership with national public health authorities and development partners. It’s anticipated that an increasing number of our COVID-19 emergency response operations will address the mental health needs of populations at risk, including frontline health workers. More broadly, addressing mental health is an important component of the Bank’s efforts to achieve universal health coverage , as an imperative for human capital development. Examples include the Liberia Supporting Psychosocial Health and Resilience Project, which is working to improve long-term psychosocial health and resilience, and the Afghanistan System Enhancement for Health Action in Transition Project, which included delivery of mental health services as part of the Basic Package of Health Services.
Delivery of mental health services is essential to achieving universal health coverage. Investing in the mental health and resilience of frontline health workers must also be part of a comprehensive response to COVID-19.


Join the Conversation
Dr./Ms. Dutta The American Academy of Experts in Traumatic Stress (www.AAETS.org) publishes the Journal of the American Academy of Experts in Traumatic Stress. The Academy is interested in publishing this article in its special edition on COVID-19. Please let me know if you will give permission for the Academy to publish this article. Of course, the appropriate citations will be included with... the article. Thank you for your consideration. Brad Lindell, Ph.D. Editor
Read more Read less