 A doctor reads a chest X-ray at the Marien Ngouabi Occupational Health Center in the city of Xai-Xai in Gaza Province. Photo: Kavita Watsa
A doctor reads a chest X-ray at the Marien Ngouabi Occupational Health Center in the city of Xai-Xai in Gaza Province. Photo: Kavita Watsa
People have been traveling from present-day Mozambique to work in neighboring South Africa’s mines for over 150 years. While conditions for workers have improved since the early days when such migrants were exploited, they continue to be under-served and neglected.
One manifestation of this neglect has been poor health outcomes for miners and ex-miners who end up experiencing high rates of tuberculosis (TB) and occupational lung disease , often undetected and untreated. These poor health outcomes also transfer to the sending community, from which the worker comes and returns. HIV infection rates are also significantly high in these groups, making negative health consequences of lung infections even greater.
Neglect and adverse health outcomes are also linked to poor working and living conditions, lack of access to adequate health information, and timely diagnostic and follow-up services, compounded by a distorted health risk perception among miners.
Health screening for vulnerable migrants
The World Bank and the Government of Mozambique, through the Regional Southern Africa TB and Health Systems Support Project (SATBHSSP, FY17-24), have been supporting health screening of vulnerable migrants and providing vital diagnostic services at border cross-points and in their communities.
In Mozambique, the International Organization for Migration (IOM) was contracted by the Mozambican Ministry of Health (MISAU) to manage a newly established occupational health center (OHC) in Ressano Garcia on the border between Mozambique and South Africa, and two OHCs in Xai-Xai and Mandlakaze, which have to send communities of migrant workers.
These centers successfully detect occupational health conditions through specialized services and innovative approaches to help reach the most vulnerable and mobile populations. IOM will eventually hand over the management of these three centers to MISAU, which is committed to providing staff and continued quality health service delivery through financing from the state budget or other health sector partners after the SATBHSSP closes in December 2023.
Diseases know no borders – Cooperation is key
Screening at border cross-points is particularly important for communicable disease control in Southern Africa, as TB incidence is disproportionately high among miners and their communities. In South Africa, TB incidence has historically been four to seven times higher among miners and ex-miners than in the general population.
The largest number of migrant miners from Mozambique cross the border at Ressano Garcia, located on the Maputo-Pretoria railway and highway, just across the border from Komatipoort in South Africa.
There, the IOM-managed screening OHC is just a few steps away from the office of TEBA, the recruitment agency that manages the contracts of miners seeking to work in the South African mines. Each year at TEBA, IOM staff encourage thousands of miners to undergo specialized medical screening, hoping to catch and stop the spread of disease and help the miners. Felix Nandza, who has worked in the South African mines for 25 years, leaving his family behind in Maputo, is one such miner who IOM has screened.
Working conditions in the mines increase the risk of getting or spreading TB. Poor ventilation and inadequately controlled exposure to silica dust damage the lungs and make them susceptible to silicosis, a high-risk factor for TB. Being HIV-positive also increases the risk of becoming infected with TB and developing active TB, which can spread further. In sending communities, dwelling places can be poor, overcrowded, and lack ventilation, allowing the broader spread of TB and other communicable diseases when workers return from the mines.
Although the IOM has worked closely with TEBA, not all miners who renew contracts at TEBA are screened, as many fear that if they are diagnosed with an illness, employers will dismiss them from employment. However, with IOM's intensified efforts and outreach in 2022-2023, the number of miners who were not screened has been falling, from 59% in June 2022 to 21% in March 2023. Between May 2022 and March 2023, 10,307 miners were screened out of the 13,825 who renewed their TEBA contracts.
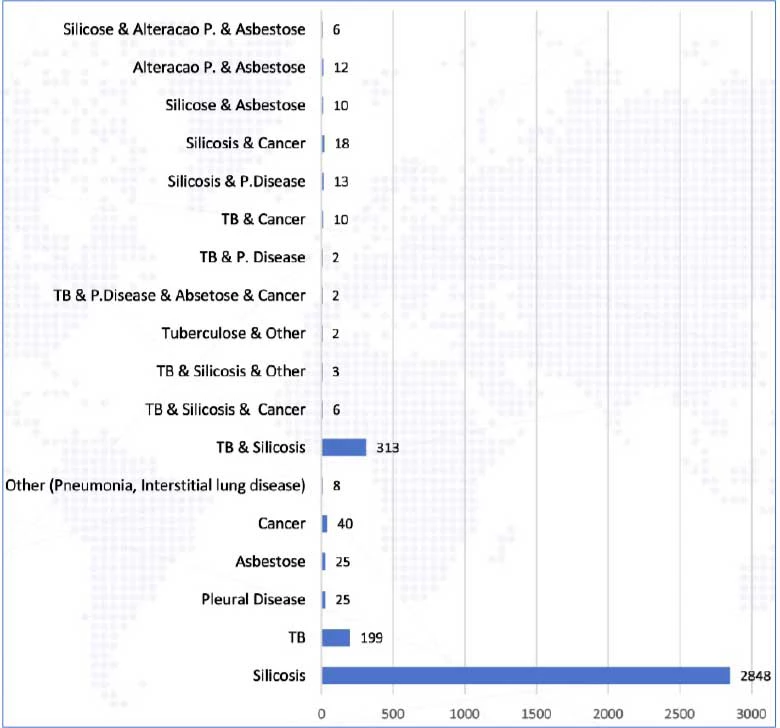
Lung disease is diagnosed with the help of chest radiographs (CXRs), and from January 2022 to March 2023, the three OHCs managed by IOM found 3,542 miners with abnormal CXRs (Figure 1). Approximately 80% showed silicosis, the most found condition; 6% showed TB, and 9% were TB associated with silicosis. Overall, the TB-positive rate was around 2% among all those screened at these centers, which is high compared to the general population.
Figure 1: Distribution of CXRs with compatible lung disease from the three OHCs (sample from January 2022 – March 2023)
Supported by the SATBHSSP, the government has been working with IOM to reach communities with vulnerable populations of miners, ex-miners, and their families in 13 districts in Inhambane and Gaza provinces. Between October 2022 and March 2023, 6,614 people were screened for TB at the community level, of which 7% were diagnosed.
This approach entails systematic screening of a target population for active (not latent) cases of TB in migrant-sending communities through community health workers, local health screening campaigns, and collaboration with traditional healers and leaders. Through IOM's targeted community-level active case-finding approach, around 50% of new TB cases detected are miners, ex-miners, and other migrant workers traveling to and from South Africa, while the remaining 50% are other community members.
IOM has also worked to ensure adherence to TB treatment among miners and ex-miners and performs screening of household contacts with on-site sputum collection and HIV testing, Directly Observed Therapy in the community (DOT-C), and refers and supports patients to access health facilities.
Cross-border collaboration
Another part of the project’s aim is to assist with compensation for miners and ex-miners, which has been a laborious process. There has been steady progress. Through the OHCs, miners and ex-miners with eligible illnesses can submit requests for medical compensation to the South African Medical Bureau for Occupational Diseases (MBOD) and the Compensation Commissioner for Occupational Diseases and receive payment in Mozambique.
Further collaboration and progress have been seen in mine regulations and inspections, accelerated by the SATBHSSP with technical support from the African Union Development Agency – New Partnership for Africa’s Development (AUDA-NEPAD). However, as with compensation, much more remains to be done to ensure mobile populations at risk and vulnerable to TB and occupational diseases receive assistance.
The SATBHSSP is active in four countries: Lesotho, Malawi, Mozambique, and Zambia, with the involvement of two regional entities – AUDA-NEPAD and the East, Central, and Southern Africa Health Community (ECSA-HC). As the closing date of the project approaches, a look back at the results achieved so far reveals substantial progress in serving the targeted, neglected community.
One of the critical indicators for the project—the number of miners and ex-miners successfully screened for occupational lung diseases—has already met its target, with 256,174 miners and ex-miners screened across the four countries .
Countries are ramping up efforts to detect active TB cases in communities, including in hard-to-reach areas, to make up for time lost during the COVID-19 pandemic, which severely affected the provision of health services in most countries. We will report more results when the project closes in December 2023.








Join the Conversation