 Au sein de la région MENA, le Maroc est un exemple de pays qui saisit l'occasion de réformer son système de santé.
Au sein de la région MENA, le Maroc est un exemple de pays qui saisit l'occasion de réformer son système de santé.
Last year, we wrote a blog and a policy note discussing the potential challenges to health systems in the Middle East and North Africa (MENA) as countries responded to COVID-19. We anticipated that COVID-19 would exacerbate the preexisting weaknesses in MENA health systems, and we recommended that countries consider implementing health financing reforms to improve sustainability and equity; strengthen health information systems to enable a proactive response; and improve the flexibility of service delivery to minimize service disruptions. Over a year later, what has happened to essential health services and health systems in MENA countries?
Significant disruptions in essential health services
COVID-19 significantly disrupted essential health services in MENA. According to two rounds of a pulse survey conducted by the World Health Organization between May-September 2020, 74% of countries reported disruptions to communicable disease treatment, 73% reported disruptions to immunization, and 38% reported disruptions to non-communicable disease treatment. While the situation has improved since then, 45% of countries still report disruptions to communicable disease treatment and 28% to non-communicable disease treatment. Despite limited data availability, evidence from countries with data such as Tunisia, Oman, and Qatar also demonstrates the rise in excess deaths, reflecting mortality that was not attributed to COVID-19 due to low testing as well as deaths resulting from foregone care for other conditions.
Countries in the region have reacted to this shock, but the adoption of measures to foster flexibility and equity in health systems has remained low. According to the same pulse survey, 59% of countries highlighted the need to triage patients and leverage community health, or move toward home-based care. And less than 40% have reported using telemedicine, extending prescription validity, or recruiting additional staff.
High frequency monitoring surveys conducted by the World Bank demonstrate the impact at a population level: During the pandemic, about 40% of the population who needed medical attention did not receive timely care in Djibouti, Iraq, and Tunisia. In the first half of 2020, half of children in Morocco were not able to access health services, which can have persisting intergenerational effects on human capital. As can be expected, the situation is even worse in fragile and conflict-affected settings, such as Yemen and West Bank and Gaza.
From crisis to reform: An unseized opportunity
A pandemic, coupled with political and financial instability, is perhaps not the best time to start implementing structural health systems reforms. Yet, the shock of COVID-19 demonstrates the need for improving the equity, flexibility, and resiliency of health systems. An example of a country that is seizing the moment to reform its health system is Morocco, where a set of ambitious reforms announced in July 2020 are currently being implemented. The reforms include the consolidation of fragmented health insurance schemes, the extension of financial coverage to over 11 million additional people in need, as well as moving towards a patient-centered, family medicine model. These reforms will assist Morocco in strengthening the resiliency of its health system in combatting future pandemics and reaching universal health coverage.
Constrained fiscal space: Bottleneck to an ambitious response
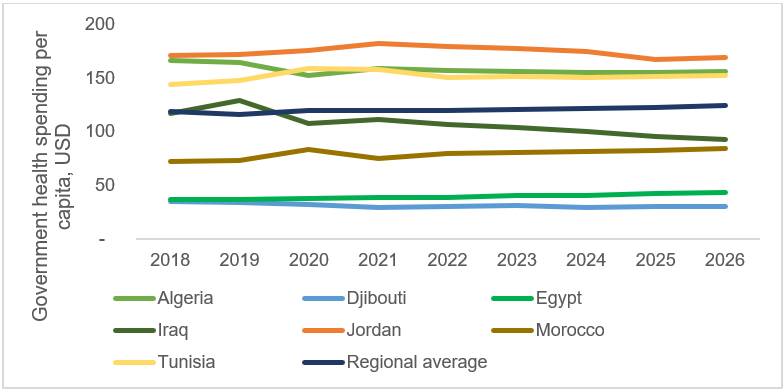
MENA countries have seen a 5.3% real GDP per capita decline in 2020, and real government revenue has declined by 24%. This macroeconomic context implies that even if countries plan to introduce bold health system reforms, they are fiscally constrained in doing so. Recent financing projections for a set of low- and middle-income MENA countries demonstrates that in most settings, government spending for health will not bounce back to its pre-pandemic levels in most countries. Unless governments significantly increase the share of health in the general government budget, it will be difficult for MENA countries to undertake structural reforms to improve equity and flexibility.
pre-pandemic share of health budget in the general government budget constant in the next five years.
Bank response: From recovery to realignment to reimagining
Most MENA countries have vaccinated below 10% of their populations, highlighting the long path to full recovery and the need to remain vigilant as new variants continue to appear. In the past year, the Bank has provided financial and technical support to 10 countries in the MENA region to respond to the COVID-19 crisis, helping close significant resource gaps in shoring up surge capacity, as well as strengthening the health system. Today, the Bank is providing financial support to Lebanon and Tunisia for the purchase and deployment of COVID-19 vaccines, with additional projects being prepared in other countries. These projects also present an entry point to reimagining pandemic-ready health systems in the region, from surveillance to sustainable financing to flexible service delivery. The Bank will continue to offer technical and operational support to countries in MENA as they move from recovery to realignment and reimagining their health systems.



Join the Conversation